Based on Your Reading:
Get Your Free Mesothelioma Guide

Find a Top Mesothelioma Doctor

Access Help Paying for Treatment

Peritoneal mesothelioma is a rare cancer affecting the lining of your abdominal cavity, or peritoneum. Inhaling or ingesting asbestos fibers can cause abdominal mesothelioma. Chemotherapy is the most common treatment. About 65% of peritoneal mesothelioma patients live at least 5 years.
Written by Dr. W. Charles Conway • Edited By Walter Pacheco
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Asbestos.com. (2024, May 3). Peritoneal Mesothelioma. Retrieved May 6, 2024, from https://www.asbestos.com/mesothelioma/peritoneal/
"Peritoneal Mesothelioma." Asbestos.com, 3 May 2024, https://www.asbestos.com/mesothelioma/peritoneal/.
Asbestos.com. "Peritoneal Mesothelioma." Last modified May 3, 2024. https://www.asbestos.com/mesothelioma/peritoneal/.
Peritoneal mesothelioma is a rare cancer of the peritoneum, the thin layer of tissue that lines the abdominal cavity. As tumors develop and grow on the peritoneum, they put pressure on vital organs and can spread to form new tumors.
Peritoneal mesothelioma is a cancer that comes from the mesothelial cell. There’s a layer of cells in the abdomen that have a lining function, regulating the passage of fluid into and out of the abdominal cavity and allowing tissues to slide easily, which is really important when the bowels move around. Peritoneal mesothelioma develops on that abdominal lining or peritoneum.
Approximately 10% to 17% of all mesothelioma diagnoses are peritoneal. Among respondents to our exclusive 2023 survey, 23% had been diagnosed with peritoneal mesothelioma. Of the estimated 1.9 million new cancer diagnoses each year in the U.S., only 300 to 500 are abdominal mesothelioma cases.
23%
The percentage of peritoneal mesothelioma diagnoses among respondents to The Mesothelioma Center’s 2023 mesothelioma patient survey.
Peritoneal mesothelioma symptoms can include stomach pain, swelling, fever and unexplained weight loss. Abdominal pain and bloating are the most common first signs. Symptoms often appear 20 to 60 years after asbestos exposure and once the cancer has already progressed to a later stage.
If you or a loved one has a history of asbestos exposure, it’s important to discuss this with your doctor. They may recommend regular screenings for mesothelioma and other asbestos-related conditions to help identify disease early.
Peritoneal mesothelioma shares common symptoms with many other abdominal disorders. An accurate diagnosis often requires a mesothelioma specialist with experience diagnosing and treating mesothelioma.
Peritoneal mesothelioma can spread or metastasize when it progresses, leading to rare and serious symptoms in other areas of the body. People may develop other symptoms if tumors spread to organs in the abdominal cavity, including the liver or intestines.
Peritoneal metastasis typically remains local or near where it originally formed. Distant metastases are rarer, occurring in 10% to 50% of stage 4 mesothelioma cases. When distant metastasis does occur, it can cause symptoms in other organs including the chest cavity and brain.
Serious but less common symptoms of peritoneal mesothelioma can be mistaken for another cancer, such as colon cancer. In our exclusive medical survey in 2023, peritoneal respondents cited anemia and bowel obstruction as serious symptoms.
There are no symptoms that are unique to mesothelioma, making it difficult sometimes to determine why a patient is experiencing them. Communicating your known history of asbestos exposure with your doctor can help raise suspicion of possible mesothelioma.
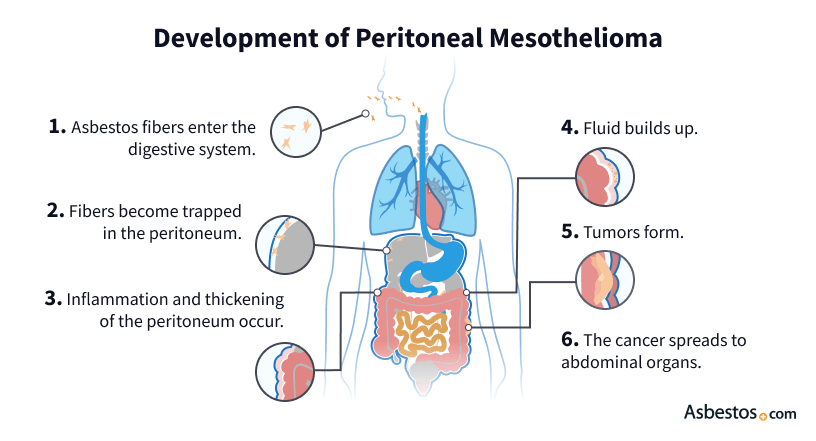
Asbestos exposure is the primary cause of peritoneal mesothelioma. Asbestos fibers can travel through the bloodstream and into the abdomen. The fibers can become trapped and cause inflammation, irritation and DNA damage. This can lead to abnormal cell growth, causing tumors to form.
Mesothelioma takes decades to develop after initial asbestos exposure. Symptoms typically appear about 40 years after exposure.
Risk factors for mesothelioma include different types of asbestos exposure, including occupational, environmental and secondary exposure. Many mesothelioma survivors were exposed while serving in the U.S. armed forces. Asbestos exposure is the primary cause of other types of mesothelioma as well.
Get Your Free Mesothelioma Guide

Find a Top Mesothelioma Doctor

Access Help Paying for Treatment

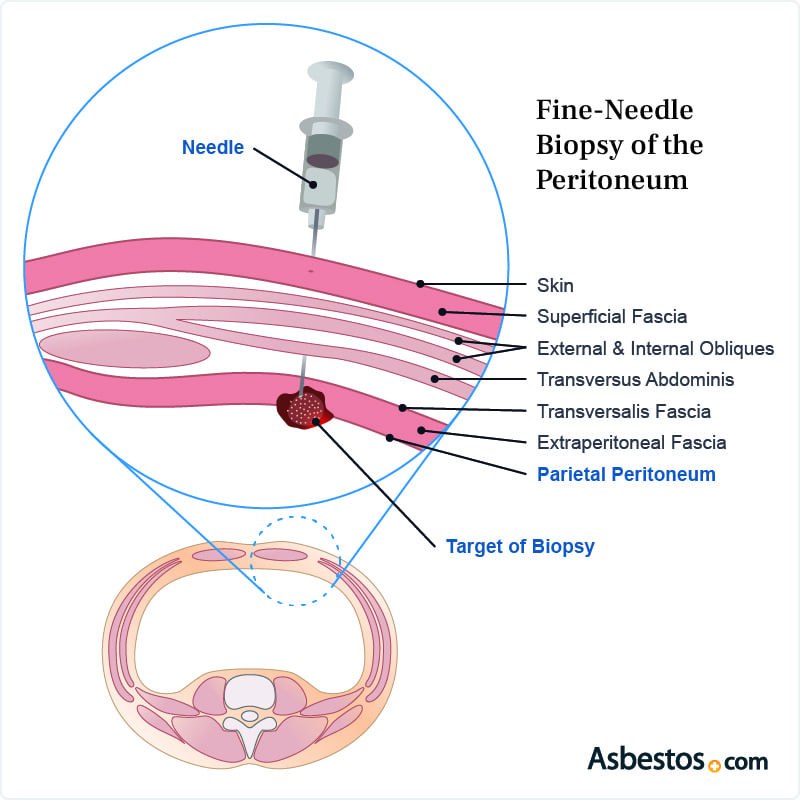
Peritoneal mesothelioma is diagnosed with a core needle biopsy or laparoscopic biopsy. A biopsy, or tissue sample, is the only way to confirm the presence of malignant mesothelioma cells.
A core needle biopsy uses a long needle inserted through the skin to collect a sample of cells from a suspected tumor. A laparoscopic biopsy involves inserting a camera and surgical instruments into the abdomen through small incisions to see inside the body and collect a tissue sample.
Collecting a sample of mesothelioma cells is essential for a proper diagnosis. Pathologists examine biopsies in a lab to identify types of cancer cells, including epithelioid, sarcomatoid and biphasic mesothelioma cell types. This information helps doctors select appropriate treatment options.
Blood tests and imaging scans are also used to help diagnose peritoneal mesothelioma. Scans are especially useful to identify tumors that have spread to nearby or distant locations in the body. The size, location and spread of tumors are all important for determining the stage of cancer.
Because peritoneal mesothelioma is so rare, most doctors and even oncologists have never seen patients with mesothelioma. As peritoneal mesothelioma survivor Sara B. told The Mesothelioma Center, “My primary care doctor told me he had never seen anyone with this disease before in his career.”
Sharing common symptoms with other diseases such as the flu and other forms of cancer also increases the risk of an initial misdiagnosis. As peritoneal cancer survivor Tamron Little told The Mesothelioma Center, “I was nauseous. I was tired all the time. It was the same symptoms I had when I was pregnant.”
I was told I had a fibroid tumor when I was pregnant. Even after my pregnancy, I was still told I had a fibroid tumor. I had surgery to remove it because of its increasing size. It wasn’t a fibroid. It was peritoneal mesothelioma.
Peritoneal mesothelioma misdiagnosis can delay treatment. The best way to get a proper diagnosis is to schedule an appointment with a mesothelioma specialist. Peritoneal specialists have the experience to ensure you get an accurate diagnosis.
The diagnostic process may seem overwhelming because of the number of tests, unfamiliar terms and procedures. A mesothelioma specialist understands this and will guide you and your loved ones through the diagnostic experience.
Tammy Frank was told an ovarian cyst was causing her abdominal pain. Surgery uncovered a much more serious problem. At the time, not many doctors could identify peritoneal mesothelioma. It took months and multiple tests to confirm. Her prognosis was grim. “I spend most of my time now helping others,” Tammy says. “I never, ever thought I’d still be here 20 years later.
There is no official staging system for peritoneal mesothelioma, so doctors use more general cancer staging to determine the disease’s progress. Doctors often use the tumor, node, metastasis system, the most widely used cancer staging system, to define 3 stages of peritoneal mesothelioma.
Using the TNM system, the stages of peritoneal mesothelioma describe the size and location of tumors and how far they’ve spread in the body. Most peritoneal patients are diagnosed at a later stage. The stage of cancer affects treatment options and helps in assessing a patient’s prognosis.
Stage 4 peritoneal mesothelioma isn’t clearly defined. Many doctors consider mesothelioma progression stage 4 when tumor spread is extensive and to distant sites throughout the body.
The peritoneal cancer index is another tool doctors use to assess tumors and help determine the approximate mesothelioma stage and appropriate treatments. PCI scores range from 1 to 39. Lower index scores mean the patient may qualify for surgery, while index scores above 20 indicate that cancer has spread too far and the patient likely won’t respond well to surgery.
Chemotherapy is the most-used treatment for peritoneal mesothelioma. The most effective treatment option is a multimodal therapy approach that incorporates cytoreductive surgery to remove tumors and hyperthermic intraperitoneal chemotherapy. HIPEC involves a multidisciplinary team of surgical oncologists, medical oncologists and other experts. Not all peritoneal mesothelioma patients qualify for this procedure.
Related Videos:
The treatment options your doctor recommends for you will depend on your stage, tumor cell type and overall health. Other treatment options for peritoneal mesothelioma include immunotherapy and surgery. Enrolling in a clinical trial can also give mesothelioma patients access to the latest treatment regimens and innovative new therapies.
Patients who aren’t good candidates for HIPEC with surgery can undergo chemotherapy as a standalone therapy. Chemotherapy delivered throughout the bloodstream is called systemic, while delivery to the abdominal cavity is called localized.
Systemic chemotherapy has a response rate of about 30%. Chemotherapy delivered directly to the peritoneum without surgery has a higher response rate of 47%.
and spread of cancer. The effective chemotherapy drugs for peritoneal mesothelioma include carboplatin, cisplatin, gemcitabine, paclitaxel and pemetrexed.
Doctors perform cytoreductive surgery, called a peritonectomy, to remove as much cancer as possible from the abdominal cavity. Then they infuse heated chemotherapy into the abdomen before the surgery ends. Heating chemotherapy and applying it after surgery increases the chemotherapy response rate to 84.6%.
HIPEC surgery has shown significant promise in treating peritoneal mesothelioma patients. A recent study in the Journal of Clinical Haematology reported that more than 80% of the patients who underwent HIPEC and continued localized chemotherapy lived 5 years or longer.
93%
The percentage of eligible patients among respondents to The Mesothelioma Center’s 2023 survey who underwent HIPEC surgery.
Doctors only perform this procedure on a case-by-case basis. HIPEC surgery is typically the recommendation only for younger patients in good enough overall health to tolerate the intensive 12-hour procedure and recovery. About 54% of peritoneal mesothelioma patients who responded to The Mesothelioma Center at Asbestos.com’s survey were eligible for HIPEC surgery.
Peritoneal mesothelioma patients I speak with commonly ask about the HIPEC procedure. We can help answer their questions and match them to specialists who can assess if it’s the right treatment for them.
Immunotherapy uses drugs that help the body’s immune system fight cancer. Because peritoneal mesothelioma is so rare, data from clinical trials is limited. Research has produced mixed results, but some studies indicate that immunotherapy may be useful in some cases of peritoneal mesothelioma.
The U.S. Food and Drug Administration hasn’t yet approved immunotherapy for peritoneal mesothelioma. The agency has approved it to treat pleural mesothelioma.
Many peritoneal mesothelioma patients receive palliative care to control symptoms and improve their quality of life. Palliative care can include procedures to reduce pain and other symptoms. This includes draining excess fluid from the abdomen (paracentesis), HIPEC and surgery designed to reduce symptoms.
Palliative care specialists can prescribe medications to control pain and mesothelioma complications. They may also refer patients to physical or occupational therapy or recommend complementary therapies to improve quality of life.

The prognosis for peritoneal mesothelioma is generally poor for patients who don’t qualify for surgery, which can significantly improve survival. For example, more than 50% of peritoneal patients who undergo surgery with HIPEC live more than 5 years. Those who undergo HIPEC, post-operative chemotherapy and long-term chemotherapy have a 5-year survival rate of 75%.
Everyone is different. No one can simply look at a diagnosis of mesothelioma and tell you what your life expectancy is.
Individual peritoneal mesothelioma prognosis and survival varies depending on several factors. These include the stage at which the cancer is detected, the specific mesothelioma cell type the person has, the treatments they choose in consultation with their doctor, any coexisting conditions they may have and their overall health.
Peritoneal mesothelioma survivors are now living longer than ever before. Statistics do show, however, that the life expectancy of peritoneal mesothelioma without any treatment is only 6 months. People who don’t qualify for surgery live about 13 months with chemotherapy alone.

Peritoneal mesothelioma is rare and difficult to treat, so it’s important to find care from an experienced mesothelioma specialist. In selecting top mesothelioma doctors to feature, The Mesothelioma Center rigorously vets specialists.
We look for doctors who practice at the top cancer centers in the U.S. and have experience in working in multidisciplinary teams. Their research and publications in medical journals are also reviewed.
Cancer hospitals with a mesothelioma treatment center offer mesothelioma specialists and an experienced multidisciplinary treatment team. They also offer mesothelioma clinical trials and a full range of support services for patients and their families.
Experience matters when treating mesothelioma. However, few doctors and hospitals have experience treating peritoneal mesothelioma. It’s important to try to find a top treatment center to ensure you have the best possible outcomes.
Unfortunately, there is currently no cure for peritoneal mesothelioma or any other type of mesothelioma yet. Research is ongoing to find better, more effective treatments.
Currently, HIPEC with cytoreductive surgery offers the best outcomes, increasing lifespan more than 5 years. Research has shown that combining HIPEC, post-operative chemotherapy and long-term chemotherapy works best. About 75% of these patients lived longer than 5 years.
Early detection of mesothelioma has a significant impact on treatment outcomes and an increased chance of long-term survival. People with a history of asbestos exposure who show signs of the disease should seek an experienced peritoneal mesothelioma specialist.
Life expectancy with peritoneal mesothelioma varies from person to person. Without treatment, median survival is 6 months. However, the overall 5-year survival rate for peritoneal mesothelioma is 65%. This percentage increases to 75% with surgery, HIPEC, post-operative chemotherapy and long-term chemotherapy.
Some peritoneal mesothelioma survivors have lived for decades after treatment — well beyond the average life expectancy. With ongoing research into new emerging treatments, experts predict the life expectancy for this cancer to increase.
Yes, according to a 2020 study, about 12% of peritoneal mesothelioma patients who undergo aggressive treatment experience complete remission. Partial remission is also possible.
Remission isn’t the same as a cure. Doctors continue to monitor patients because cancer can return after entering partial or complete remission.
Managing a cancer diagnosis is a challenging experience for patients and their loved ones. There is no one right way to cope with mesothelioma. Every individual experience is different.
Tips for Managing a Cancer Diagnosis
It’s important for cancer patients to remember they’re not alone. Many resources are available. Cancer treatment is constantly evolving, and survival has significantly improved for peritoneal mesothelioma thanks to advances in treatment.
Asking your doctor questions about peritoneal mesothelioma can help in managing a diagnosis.
Peritoneal Mesothelioma Questions
Healthcare communication at these appointments often falls on caregivers. Be prepared ahead of medical appointments to ask questions and communicate clearly with doctors. This can help families feel informed and empowered.

Have a question? Contact one of our Patient Advocates and get the answers you need.

Connect, share stories and learn from the experiences of others coping with mesothelioma in one of our support groups.

We help support charities, hospitals and awareness groups working to help people impacted by asbestos and cancer.
Your web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
