Based on Your Reading:
Get a Mesothelioma Treatment Guide

Find a Top Mesothelioma Doctor

Access Help Paying for Treatment

Immunotherapy, vaccine therapy and cryotherapy are new emerging treatments for mesothelioma. The combination of Opdivo and Yervoy were approved by the FDA in 2020 for first-line treatment of malignant pleural mesothelioma. This makes it the first drug regimen approved for mesothelioma in 16 years.
Written by Sean Marchese, MS, RN • Edited By Walter Pacheco • Medically Reviewed By Dr. Daniel Landau
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Marchese, S. (2024, February 2). New Mesothelioma Treatments. Asbestos.com. Retrieved April 24, 2024, from https://www.asbestos.com/treatment/emerging-treatments/
Marchese, Sean. "New Mesothelioma Treatments." Asbestos.com, 2 Feb 2024, https://www.asbestos.com/treatment/emerging-treatments/.
Marchese, Sean. "New Mesothelioma Treatments." Asbestos.com. Last modified February 2, 2024. https://www.asbestos.com/treatment/emerging-treatments/.
Traditional treatments help people with mesothelioma cancer live longer with a better quality of life. However, there is still much room for improvement. Recent research has led to several emerging treatments for mesothelioma.
For patients who don’t respond to standard therapies, experimental new treatment options may provide a source of hope. We don’t yet have a cure for mesothelioma. But doctors have developed new treatments in recent years that improved survival.
Emerging mesothelioma treatments have identified new targets against mesothelioma cancer. Many of these new treatments also work best when paired with traditional options. Examples include immunotherapy, vaccine therapy and gene therapy.
Immunotherapy for mesothelioma influences immune cells to identify and destroy cancer cells. Mesothelioma immunotherapy is an intravenous medication. It is approved for pleural mesothelioma, and peritoneal patients may access it through trials.
Immunotherapy provides several benefits over chemotherapy. It uses your natural immune cells to fight cancer. It often involves fewer and less severe side effects, such as rash, cough or intestinal issues. Checkpoint inhibitors such as pembrolizumab (Keytruda) are some of the latest developments.
The U.S. Food and Drug Administration also approved nivolumab (Opdivo) and ipilimumab (Yervoy) for mesothelioma. Doctors often prescribe immunotherapy alongside chemotherapy as part of a multimodal treatment plan. Newer immunotherapies are available through clinical trials.
Get a Mesothelioma Treatment Guide

Find a Top Mesothelioma Doctor

Access Help Paying for Treatment

Vaccine therapy is a new mesothelioma treatment option that involves immunotherapy. A cancer vaccine instructs your immune system to make antibodies against cancer cells. Like how the flu vaccine prepares your body to identify and attack the influenza virus. Mesothelioma vaccines are still in clinical trials.
In a trial, patients who received the WT1 vaccine had a median overall survival of 21.4 months compared to 16.6 months for those who received a placebo. Doctors are also testing vaccines with immunotherapy drugs such as Opdivo.
Photodynamic therapy uses photosensitizing drugs that react to a particular light. When stimulated, these drugs kill cancer cells and prevent metastasis. This treatment also lacks substantial side effects, which could help improve a patient’s quality of life.
Low-dose photodynamic therapy (L-PDT) combined with immunotherapy has been studied in mice. The results showed a complete mesothelioma regression in 37.5% of animal test subjects.
Cancer cells carry DNA like all healthy cells in the body. However, mutations or defects in DNA cause normal cells to transform into cancerous tumors. Gene therapy for mesothelioma attempts to repair or replace genes in the DNA that lead to cancer.
One of the latest developments in the treatment of mesothelioma with gene therapy is gene transfer. For example, replacing the BAP1 gene leads to tumor suppression. Transferring “suicide genes” into cancer cells could allow certain chemotherapies to work better.
Epigenetic therapy for mesothelioma focuses on how DNA expressions translate to changes in the body. For example, age, environment and lifestyle cause our DNA to express genes differently. Current emerging mesothelioma treatments include epigenetic targets UHRF1 and inflammation biomarkers.
Epigenetic therapies might reverse asbestos damage and promote regular DNA gene expression. A 2021 study demonstrated that epigenetic changes affect pleural mesothelioma survival rates. Phase II clinical trials are ongoing for tazemetostat. It targets the BAP1 enzyme involved in epigenetic regulation.
Anti-angiogenic drugs are a mesothelioma treatment that targets blood vessel growth in tumors. Angiogenesis is the process of growing new blood vessels. They supply tumors with the oxygen and nutrients that allow cancer to grow and spread. By stopping this process, anti-angiogenic drugs can prevent tumor development and metastasis.
One new mesothelioma treatment option is bevacizumab (Avastin). Some of Avastin’s side effects are potentially severe, such as blood clots, hemorrhaging or low white blood cell counts. Scientists are still working to decrease these effects. Cediranib is another new mesothelioma treatment that targets tumor angiogenesis
Cryotherapy uses freezing temperatures to kill cancerous cells. This targeted therapy reduces tumor size and improves mesothelioma symptoms.
Because cryotherapy targets a specific location, it’s less invasive and produces fewer side effects. In a 2020 study, researchers used cryotherapy to provide chest pain relief for a median of five weeks.
Although it is a new treatment for mesothelioma, virotherapy has existed as a cancer treatment since the 1950s. Viral immunotherapy and viral vector therapy use viruses to infect and destroy cancer cells. Oncolytic viruses destroy cancer cells through aggressive replication.
Viral vectors are modified viruses. They deliver immunotherapy drugs or gene therapy, such as the p53 gene, into tumor cells. The viral activity also triggers the immune system to respond and attack the cancer site. Some virotherapy studies for mesothelioma have demonstrated improved disease response and overall survival.

Multimodal therapy is the term for combining multiple treatments. Combining mesothelioma surgery and chemotherapy is more effective than either treatment alone. Combining traditional and emerging therapies will become the new gold standard.
Combining therapies controls tumor growth and cancer spread with numerous techniques. Post-surgical radiation for mesothelioma can kill cancer cells left behind from surgery. However, patients are also subject to side effects from multiple treatments in a multimodal plan.
Emerging cancer treatments give physicians more options. Tumor Treating Fields helped control tumor growth in clinical trials. The FDA approved TTFields for mesothelioma in 2019, and it is now part of a standard multimodal plan with chemotherapy.
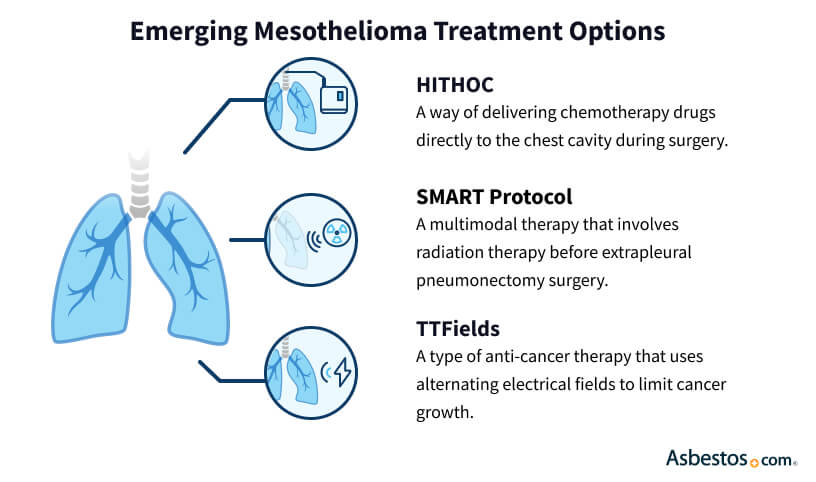
Hyperthermic intraperitoneal chemotherapy involves heated chemotherapy circulated through the abdomen during surgery. A similar technique kills cancer cells throughout the thoracic cavity.
Another emerging treatment option is surgery for mesothelioma after radiation. It is also known as the SMART protocol. SMART is a multimodal therapy that involves radiation therapy before extrapleural pneumonectomy surgery.
People access new and emerging mesothelioma treatment options through clinical research trials. Clinical trials are limited to specialized treatment centers. Patients must also pass an eligibility checklist to ensure their safety.
Examples of eligibility requirements for a clinical trial include cancer stage, cell type, tumor location, overall health and previous treatment history. Patient Advocates at The Mesothelioma Center can help patients interested in emerging therapies find eligible clinical trials and treatment centers in their area.
One of the first steps in participating in a clinical trial is speaking with your mesothelioma specialist. If you’re unsure how to enroll in clinical trials in your area, The Mesothelioma Center Patient Advocate team can match you with local studies.
Many patients benefit from a clinical trial when other options have failed. In a research study you’ll have access to the newest medications. Study sponsors will often cover the entire cost of the experimental treatment. If at any point during the study you wish to drop out, or you aren’t receiving a benefit, your doctor will switch you to a standard-of-care treatment.
Specialists offer the newest treatment options available. They have the knowledge and experience to diagnose asbestos-related illnesses quickly and accurately. They also know the best multimodal treatment plans for each patient’s diagnosis.
Finding a mesothelioma specialist can be challenging. Getting a second opinion or referral can make a significant difference. Specialists are involved in the latest mesothelioma research using cutting-edge technology.
Emerging mesothelioma therapies and clinical trials are available at specialized cancer centers. These facilities offer new mesothelioma treatment options.
The teams at top mesothelioma centers include world-renowned oncologists, surgeons and other experts. At most centers, these experts meet to deliberate the best mesothelioma treatment options for each patient.
The U.S. Food and Drug Administration’s approval process involves several checks to ensure safety and effectiveness.
Pharmaceutical companies must prove that their drug’s benefits outweigh its risks. The FDA has a five-step approval process for new drugs. Researchers prove safety during the discovery phase and in preclinical research. Human participants join the clinical testing phase. Then the FDA reviews trials and conducts post-market monitoring for safety.
Criteria for drug quality, safety and effectiveness are set by the FDA’s Center for Drug Evaluation and Research. The CDER oversees these standards for prescription and over-the-counter drugs. Other FDA centers test safety across medical devices, food, veterinary drugs and tobacco products.
Your web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
